WP_Post Object
(
[ID] => 1158
[post_author] => 1
[post_date] => 2018-05-09 12:20:07
[post_date_gmt] => 2018-05-09 18:20:07
[post_content] => The University of Regina Cougars Women's Basketball team was taking on their rivals, the University of Saskatchewan Huskies, at home in the USPORT Final 8 semifinals after beating them the week prior in the Canada West final. They were surrounded by 2,411 fans, who had packed the stands, the overflow watching from the upstairs track. A player couldn't ask for a better atmosphere: the crowd hanging on to every pass and shot, roaring for every Cougars basket and steal.
With two minutes to go, the game was tied at 68. The Huskies hit back-to-back three-pointers to take a 74-68 lead. Although they fought, urged on by their fans, the Cougars could come no closer than 74-71.
When the final buzzer sounded and the Huskies rushed the court in victory, the air was thick with disappointment, from the tears of the players as they made their way to the dressing room, to the fans who slowly filed out of the packed stands.
"You know, you work all year for that moment, and then it's gone in the blink of an eye," says Charlotte Kot, captain and fifth-year player in 2017-18.
"You know, you work all year for that moment, and then it's gone in the blink of an eye," says Charlotte Kot, captain and fifth-year player in 2017-18. "I gave myself that night to be upset about it. You're kind of grieving the loss of the goal you have all year. When I woke up, though, it was still game day. I knew I would regret it in the future if I didn't enjoy that last game."
The Cougars had a competitive fire within them that wouldn't allow them to sit back in the bronze medal game, and they beat the McGill Martlets in a hard-fought match 66-63.
"It's a strange sensation, because we were 36-5, won our conference and finished third in the country and honestly, the season was a bit of a disappointment," says head coach Dave Taylor, signifying just how high of a standard this team sets for itself. "It's a really good statement about where we are as a program and a team."

Graduating Cougars player, Charlotte Kot. (Photo by University of Regina Photography Department.)
There's a magic about this program - something that is difficult for alumni or coaches to put into words - but a wide variety of factors have come together to create a product that draws people to it, including recruits, top-level coaches and fans.
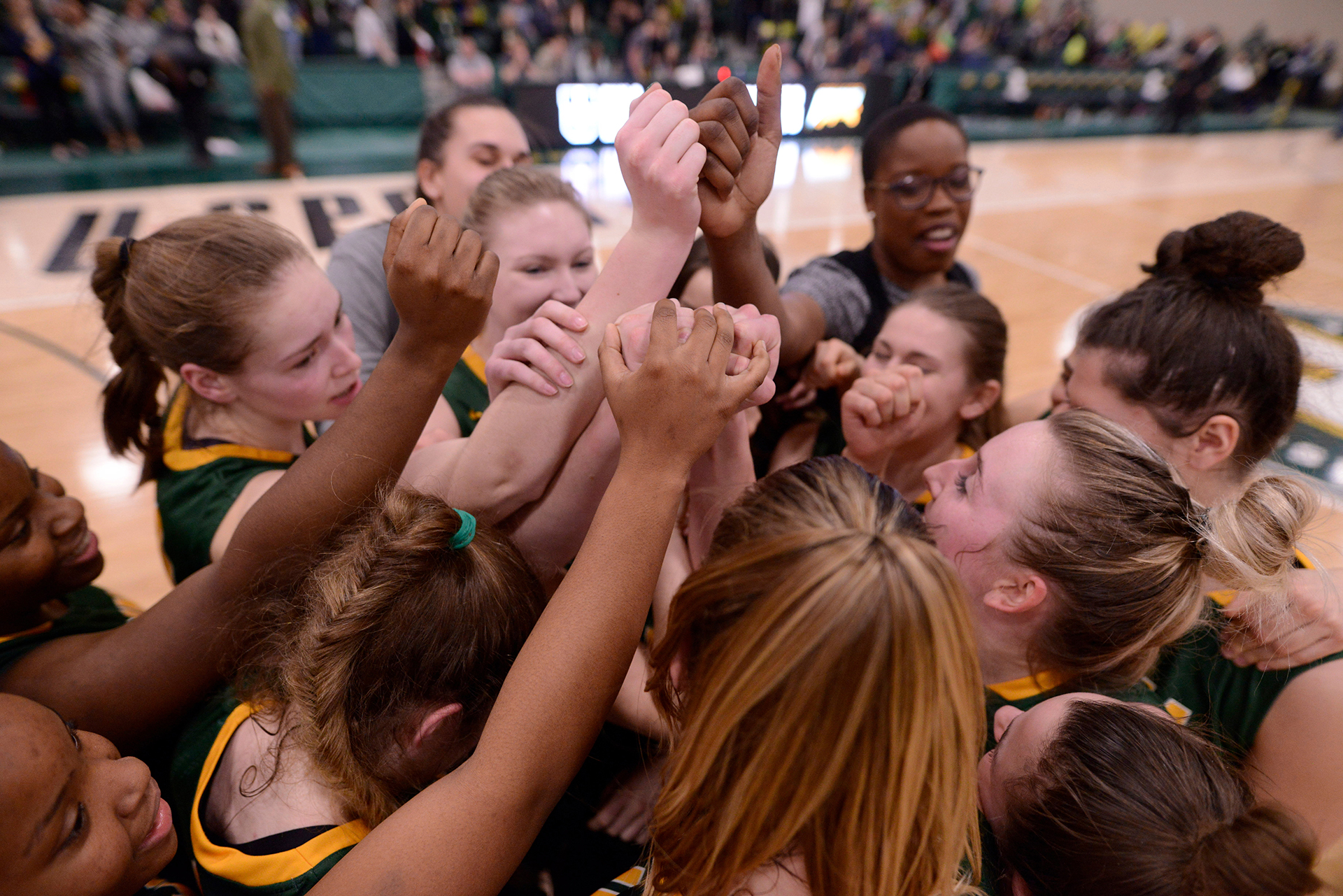
The Cougars celebrate another medal in a national championship, winning bronze at the 2018 USPORT tournament in Regina. (Photo by Arthur Ward)
Over the past 20 years, the Cougars have finished only one season without a winning record. This is a team that, since 1968, has played in the national university championship 19 times, advancing to the final championship game on six occasions. It is one of the best programs in Canada.
The success of the program can be attributed to a number of factors. Alumni and coaches have a slightly different view on what has advanced the program to the position sustained success it has seen. Perhaps it is the high calibre of local players developed through the Regina club and school programs. It could be the emphasis placed on recruiting. Or maybe it's simply the mindset of maintaining a high standard of excellence. Together, the elements have created a product that draws the support of the community and makes this one of the most respected programs in Canada.
Over the past 20 years, the Cougars have finished only one season without a winning record.
The Centre for Kinesiology, Health and Sport (CKHS) gym that was packed to the rafters in the 2018 championship semifinal game is a far cry from the early days of the program, and shows the level of growth over the years.
Sue (McKenzie) Burns BEd'81, MEd'02, who played for the team from 1977 to 1981 says, "The fans would strictly be our parents, and if you had a boyfriend, there'd be a boyfriend there too."
When women first started playing basketball at the University from the 1940s through the 1960s, it was recreational, emphasizing participation and exercise, says Jim Pitsula, a retired history professor from the University of Regina who also became one of the Cougars' most avid fans.

Sue (McKenzie) Burns. (Photo by Trevor Hopkin)
The first year the team donned uniforms as the Cougettes was in 1968-69, playing for the University of Saskatchewan - Regina Campus under head coach Sheila Ward. Their green uniforms were made off-site, and the armholes were so small, the women couldn't raise their arms, says Irene Wallace, one of the original Cougette alumnus. "In the locker room after practice we ended up taking scissors and making larger arm holes so we could actually wear them."
Original Cougettes (left to right) Linda (Vail) Dodd BEd'74, Irene Wallace BEd'71, Ruby (Werhun) Patrick BEd'72 and and Laurie (Woods) Burgess BEd'70.
(Photo by Trevor Hopkin)
The developing history of Cougar women's basketball has continued to reflect the University, as it has grown from a completely local program to one that is recognized internationally.
Each head coach has continued to move the program forward. When Sue Higgs, a Department of Physical Education faculty member, began coaching the team in 1971, she began to revolutionize the team and women's sport.
"I think she was a little bit ahead of her time in terms of, let's take these young women and really maximize their physical potential, in addition to teaching us so many things we didn't know about the game," says Burns, who noted that they were always in the lab doing fitness testing as well as training off the court.
After Higgs' nine-year tenure, there were two losing seasons before Sheila (Brennan) Beckie was hired. A Regina product, she had played for the University of Saskatchewan, and brought with her enthusiasm for the program, as well as a real focus on recruiting local players.
"We were losing really good athletes out of the city," says Dick White CA'89, BEd'74, who worked for the University for 34 years, including 20 as athletic director. "One of her focuses was to keep the best Regina athletes here at the start."

Sue Higgs began coaching the team in 1971 and began to revolutionize the team and women's sport. (Photo courtesy of University of Regina Archives and Special Collections.)
During her first season, there was such a lack of returning players and few players previously recruited that Beckie would have to join the players in practice to have enough bodies. Then, she successfully recruited Jackie Moore BPAS'91 of Thom Collegiate. The Cougars continued to improve, winning the Great Plains Athletic Conference (GPAC) final and going to the national championship in the 1988-89 season.
"That was kind of a turning point, I think, for the program, where it wasn't just an afterthought, but starting to be a premier program in the country."
"These young ladies really put in a lot of time on their own outside of practice time, working on their game, playing in the summers, getting into the weight room, taking their nutrition and fitness seriously," says Beckie. "That was kind of a turning point, I think, for the program, where it wasn't just an afterthought, but starting to be a premier program in the country."
After Beckie left, Debbie (Patterson) Nash coached for four seasons, but the strong group of players had graduated, weakening the program by the time Christine Stapleton was hired in 1993.
Stapleton had won a championship as a player with Laurentian University over the Cougars in 1991, and knew the type of basketball played at the University of Regina.
"The athletes were well prepared, extremely well coached, tough, fit, intelligent and sportsmanlike," she says. "They never stopped competing."
Stapleton continued Beckie's focus on recruitment, and began creating a community profile.
"I admire, especially, Sheila and Christine," says White. "They were able to recruit on the promise of, 'If you come, we will get better.' "
When Stapleton first arrived, she met with the coaches of the high school basketball teams. One of those coaches was Dave Taylor, who became her assistant coach and has been with the program ever since.
Cougars coaches (left to right) Diane Hilko, Christine Stapleton and Dave Taylor after winning the national championship and the Bronze Baby in 2001.
(Photo by by University of Regina Photography Department)
It was a struggle at first, but Stapleton recruited hard and was determined. She had played for and learned from legendary coach Peter Ennis, and brought passion, energy and confidence.
"The plan was to work hard," she says. "Build the grassroots, immerse myself in the community, and make sure that the best local talent stayed." To new players, she would say, "'So, you've come here. You're going to graduate. And you're going to be a way better basketball player. And if we win a few games as part of this agreement, then we both win.' And that's what we did."
For many years the team played in GPAC, which consisted of the University of Regina, University of Manitoba, University of Winnipeg and Brandon University. It was a tough division, but it meant the Cougars played the best teams each weekend.
"I remember a moment where, literally, Sandra Carroll, who was playing for Winnipeg, was outscoring us late in the game," says Taylor. "She'd average like 49 points a game against us. And that drove Christine and myself to where we're going, we've got to get better. Then Trena Mott BAdmin'99 came, and I call her the Pied Piper, because then Amy Mickleborough BEd'98 came, and Andrea Gottselig MEd'10, and that brought Becky Poley BA'02, Crystal Heisler BAdmin'03, BEd'09, and the group that went to our national title."
The road to that title actually began the previous year, when the Cougars lost what Stapleton calls a "gut-wrenching" CIS Championship semifinal game against the University of Calgary. "I'll never forget going back to the hotel and going, 'That's never happening again,' " she says.
The road to that title actually began the previous year, when the Cougars lost what Stapleton calls a "gut-wrenching" CIS Championship semifinal game against the University of Calgary. "I'll never forget going back to the hotel and going, 'That's never happening again,' " she says.
The next year, they once again found themselves playing Calgary in the semifinal game. Despite all of the changes they had made, and the whole shift in focus over the previous year, the coaches could hardly believe that at halftime, they found themselves down once again. They went into the locker room, walked the team through the game, tinkered with some defence, and the Cougars came back out and won the second half.
The final game was between the Cougars and the home team, the University of Alberta Pandas. The Cougars all wrote "MH" on the bottom of their white shoes, standing for "Make History." They did just that. Seven of the Cougars finished the game in double figures, and when the final buzzer sounded, they won 94-85.

The 2000-01 CIS championship women's CIS team. (Photo by University of Regina Photography Department)
As the Cougars became more successful, their fan base also grew. In 1999, the Cougars were playing the University of Manitoba in the best-of-three GPAC final. After the warmup, Stapleton and Taylor were walking toward the team room, about 40 feet down the hallway from the gym, and could hardly get through because the lineup to the gym was out the door. "Dave and I looked at each other, with big smiles on our faces, and were like, 'Can you believe this?' " says Stapleton.
Jeff Speedy, who was hired as the head coach in 2002 after Stapleton, says the city's passion for the program makes Regina one of the top places in the country to coach. "It's a special place to play, it's a special place to coach, and it's a very special program," he says.
"People hated coming there, because the sideline was packed with people, the end lines were packed with people, and the stands were right on top of you."
Phoebe De Ciman BA'03, BAHons'05 joined the team in 1998, playing for four seasons under Stapleton and one with Speedy. Like many of the alumni, she has stayed in Regina and become a leader in the community. "I was so lucky to have been part of the program when that turnaround happened, where I could really see people were excited," she says. "The support from the community was absolutely fabulous. We were packed before the guys came in. It's very unique."
The last game played in the old gym was the Canada West Championship in 2004, when the Cougars beat the University of British Columbia, in front of over 800 fans packed into the small space.
"People hated coming there, because the sideline was packed with people, the end lines were packed with people, and the stands were right on top of you," says Cymone (Bouchard) Bernauer BKin'04, BEd'09. "It was really kind of bone-chilling. You make a good play and the place erupts and the hair on your arm stands up. It was very intense and just, really, the passion for the game was electric."

Former Cougars player Cymone (Bouchard) Bernauer. (Photo by University of Regina Photography Department)
The next year, the team was creating new memories in a state-of-the-art facility after the Centre for Kinesiology Health and Sport opened. They needed to win the third game in the series to advance to the final four. The Cougars had graduated three players the previous year, one being Bernauer, who had been named the CIS Player of the Year. "We were trailing late in the game," says Speedy. "We were down six points with only five minutes left in the game, and I can still remember Jana (Schweitzer) Linner BAdmin'05, and Leah Anderson taking the game over. Basically, they were just saying, 'There's no way our careers are done today.' We won that game to even the series, and won the next day to go back to the final four."
The move to the new 2,400-seat gym meant a beautiful new team room, additional training facilities and, later, a jumbotron.
"It changed the atmosphere a little bit," says Maja Kralcacova BKin'09, who played for the Cougars from 2003 to 2009. "But it also gave the opportunity for a lot more people to watch us play."
Maja Kralcacova.
(Photo by Trevor Hopkin)
Kralcacova was one of the first international players to come to Regina. Originally from Prague in the Czech Republic, Kralcacova played her senior year of high school in Macklin, Saskatchewan, before Speedy recruited her to the Cougars.
"The team is now kind of reflecting where the U of R's going," says De Ciman. "Internationalization is growing, and you can almost say it's mirroring the University."
While the Regina community supports its local players, it also welcomes international players, making them feel like family.
"It was just incredible how people embraced me. … It was really nice, and that continued throughout all of my years," says Kralcacova, who stayed in Regina following her basketball career and recently became a Canadian citizen.
The warm welcome is because of avid fans like Gord Staseson, who Kralcacova now calls her "grandpa" for all he has done for her over the years.
"He took me under his wing, and started to help me fundraise money for Adopt-a-Cougar," says Kralcacova, who remains close friends with Staseson. "He actually raised money to bring my mom here for the (2009) CIS Championship, which was really touching, and I will never forget it."

Gord Staseson (Grandpa to former player Maja Kralcacova) hoods her at her 2009 convocation ceremony. (Photo courtesy of Maja Kralcacova)
Much of the recruiting to the Cougars, however, still remains within the city. Regina minor level and high school basketball teams continue to develop strong athletes who grow up wanting to play for the Cougars. Alumni give their time generously, coaching at various levels as they become role models in the community.
"I think we have always had the perfect storm," says Taylor. "We've been successful. Our players are great ambassadors out in the community. So there's that connection. … Local will always be the foundation of our program. The minute that changes, we're in trouble."
Thirteen years after joining the Cougar women's basketball team as an assistant coach, Taylor was made head coach in 2006.
"It's a village that builds this program," says Stapleton, noting the athletic directors, deans of Kinesiology and Health Studies, and University presidents who have supported the teams and shown up to games. "And it's a guy like Dave, who has arguably the longest tenure of anybody associated with the women's basketball program."
Taylor is quick to acknowledge the coaches that came before him as the team's builders, while he says he is committed to maintaining that excellence as guardian of the program.
For most of the past 25 years, the University of Regina women's basketball program has been in the capable hands of Dave Taylor or Christine Stapleton.
(Photo by Rae Graham)
"There have been all these moments and times where I thought there were tipping points that could have gone either way. Oftentimes, it has been having the right player with the right mindset," says Taylor, in looking back on the team's success over the years. "The players have had that competitive drive and ownership, and just pursuit of excellence where anything less is just not acceptable."
In 2013-14 and 2014-15, the Cougars had back-to-back seasons where injuries became a huge issue, leading to two seasons where the team didn't go to nationals. The summer of 2015, Charlotte Kot became the team's heartbeat, and her drive to succeed permeated the entire team. "Everybody had that attitude of, 'Okay, enough. We can't be 500. This is not acceptable,' " says Taylor. "And now, we're back on a three-year run of being in the Canada West finals."
While players like Kot will certainly never forget playing in a national championship, she says her most important memories of the weekend were not on the court. Instead, she will remember the alumni who returned for the weekend, including those such as Andrea (Gottselig) Ward and Amy (Mickleborough) Moroz, who co-chaired the 2018 championship committee.
"The thing I will remember the most about that nationals was all of the alumni," says Kot, who was awed by the packed gym watching the alumni game and the lunch with over 65 alumni present. "The people change, but they are always your family. … Once a Cougar, always a Cougar."
Crystal (Heisler) McGregor played with the Cougars from 1996-2002. Her death from cancer in 2014 brought players closer together than they had ever been.
Never was this more apparent than when Crystal (Heisler) McGregor was diagnosed with cancer in 2012. McGregor played for the Cougars from 1996 to 2002. The Cougar alumni - including both her teammates and those from teams before and after - came together to fundraise and help McGregor in her battle against cancer. When she died in 2014, they began the Crystal McGregor Memorial Scholarship in her memory.
"It drew us closer together than we've ever been, and that's the beauty of being part of a team," says Bernauer. "No matter what happens to somebody in that extended family, we all pull together, and we all show up for support."
"As tragic as it was to lose Crystal, you try to answer the question 'why?' We tried to take the love and the positive out of it," says Ward. "Crystal reconnected all alumni in a deeper and more meaningful level of team than ever before."
"It's a village that builds this program," says Stapleton.
It also demonstrated that no matter how busy life gets, the team is there past basketball. "The people are what matter," says De Ciman. "If someone needs lifting up, we'll be there. And if someone's joyful and celebrating, we'll be the first ones on the dance floor at the wedding."
While the results are important, that is only a piece of what has made this program successful.
"University athletics is part of a process of education of character development, intellectual development, social development," says Pitsula. "It is, by its very nature, part of that developmental shaping of personalities, shaping of character, preparing people for life."
That is certainly exemplified by the Cougars and the people they have become. This is a program that has not only captured the heart of the community, but also has become a reflection of it. Because, at the end of it all, while basketball has brought the Cougars community together, it is the people and relationships that forever uphold the Cougars spirit.
Over the years
1967-68
University of Regina Cougettes, a junior team, begin playing against other university's junior teams.
1968-69
Sheila Ward becomes head coach; Cougettes begin playing in the Western Canadian Intercollegiate Athletic Association.
1971-72
Sue Higgs becomes head coach.
1972-73
WCIAA splits into two divisions; Cougettes begin playing in the Great Plains Athletic Conference (GPAC).
1974
As the University of Saskatchewan - Regina Campus becomes the University of Regina, the basketball team takes a hiatus from GPAC until the 1976-77 season.
1976-77
The Cougettes appear at the GPAC final for the first time.
1978-79
The Cougettes appear at the national (CIAU) championship for the first time as the host team.
1980-81
Bernie Riffel coaches.
1981-82
Linda Dodd coaches.
1982-83
Sheila Beckie is hired as head coach on a 10-month term.
1983-84
Beckie's contract becomes permanent; the Cougettes become the Lady Cougars.
1988-89
The Lady Cougars win the GPAC final for the first time.
1989-90
Debbie Patterson is hired as coach.
1990-91
The Lady Cougars win the GPAC final; they appear in the CIAU final for the first time.
Early 90s
The Lady Cougars become the Cougars.
1993-94
Christine Stapleton is hired as head coach.
1995-96
Andrea Gottselig is named CIAU Rookie of the Year.
1996-97
Christine Stapleton is named CIAU Coach of the Year.
1998-99
Corrin Wersta is named CIAU Player of the Year; the Cougars win the GPAC final.
1990-00
The Cougars win the GPAC final and the bronze medal at CIAU Championship.
2000-01
The Cougars win the GPAC final and the CIS Championship.
2001-02
The Cougars move to the Canada West (CW) division.
2002-03
Jeff Speedy is hired as coach
2003-04
Cymone Bouchard is named CIS Player of the Year; the Cougars place first in the Final Four and second at the CIS Championship.
2004-05
The Centre for Kinesiology, Health and Sport opens.
2006-07
Dave Taylor is hired as head coach.
2007-08
The Cougars place second at the CIS Championship.
2008-09
Regina hosts the CIS Championship and the Cougars place second.
2011-12
Dave Taylor is named CIS Coach of the Year.
2012-13
The Cougars win the CW Final Four; Regina hosts CIS nationals and finishes second.
2016-17
Kyanna Giles is named U Sports Rookie of the Year.
2017-18
The Cougars win the CW Final Four; Regina hosts U Sports Nationals and finishes third.
[post_title] => A look back at the Cougars
[post_excerpt] => The University of Regina women’s basketball program has been one of the best and most enduring programs in the country.
[post_status] => publish
[comment_status] => open
[ping_status] => open
[post_password] =>
[post_name] => a-look-back-at-the-cougars
[to_ping] =>
[pinged] =>
[post_modified] => 2022-02-23 15:32:59
[post_modified_gmt] => 2022-02-23 21:32:59
[post_content_filtered] =>
[post_parent] => 0
[guid] => https://www.degreesmagazine.ca/?p=1158
[menu_order] => 0
[post_type] => post
[post_mime_type] =>
[comment_count] => 0
[filter] => raw
)
WP_Post Object
(
[ID] => 1247
[post_author] => 1
[post_date] => 2018-05-10 09:39:53
[post_date_gmt] => 2018-05-10 15:39:53
[post_content] => Irene Mosquito sits stitching beads carefully onto a pair of leather gloves lined with soft rabbit fur. Her ease with both the stitching and the noisy children surrounding her are telling. Just behind her are various pictures of other crafts that she has shared with people who enter through the doors of the Four Directions Community Health Centre every Saturday. One of the crafts stands out.
"It's called a moss bag," she says with a warm smile. "They're used for more than just keeping babies warm." Mosquito explains how the moss bags are meant to simulate a baby's life in the womb. "There is even a cord with criss-crossed threads that sits on the inside of the bag," she says. "Every criss-cross of the thread has a traditional teaching related to it."
Irene Mosquito (right) used to be a SEARCH client, now she works as a support worker at the after-hours clinic. Mosquito sits with volunteer Busi Mabhena.
(Photo by Trevor Hopkin)
Amidst the hustle and bustle of people, many of them nervous University of Regina students, Mosquito is a calm oasis. Her beautiful black hair is pulled back in a ponytail. Calling her older than most of the others here doesn't seem quite right. The term grandma seems much more appropriate because ever since she entered the room, the younger children gravitate towards her. She also has that unmistakable presence that makes certain people seem more like an elder than just elderly.
Mosquito is the support worker for SEARCH (Student Energy in Action for Regina Community Health). Started in 2009, SEARCH was the brainchild of a group of post-secondary students who wanted to get involved in a community health initiative in Regina's inner city. Their partnership with the University of Regina and the Regina Qu'Appelle Health Region led them to Four Directions Community Health Centre, a clinic that had been offering primary health care in the North Central neighbourhood for more than 20 years.
Using student and professional volunteers, SEARCH builds upon the great work that Four Directions is doing by extending the hours of service into the weekend. Professionals at the facility include doctors, social workers, counsellors, nurses, nurse practitioners, physical therapists and dieticians. Beyond offering these essential services to clients, the professionals provide mentorship to the student volunteers. This community of learning between professional mentors, student volunteers and clients is one of SEARCH's greatest assets.
Started in 2009, SEARCH was the brainchild of a group of post-secondary students who wanted to get involved in a community health initiative in Regina's inner city.
Mosquito first got involved with SEARCH because she needed its services as a client. "It did a lot for me," says Mosquito, who lives in North Central but is originally from Whitefish, Saskatchewan. "For example, for physiotherapy, I didn't have to go far, because sometimes I didn't have a vehicle."
A convenient location was only one of many benefits that SEARCH offered. "When I needed to see the doctor or the physiotherapist, I knew that [SEARCH] was there for me and that I didn't have to worry about waiting, waiting, waiting."
The convenience and the friendliness of the people at SEARCH compelled Mosquito to work there herself. Recognizing the importance of Indigenous culture, SEARCH ensures it has staff who can provide leadership and guidance in traditional ways. "I let [the clients] know that it's okay to be Indian, to use their language, because a lot of people have lost their culture in this community."
Started in 2009, SEARCH was the brainchild of a group of post-secondary students who wanted to get involved in a community health initiative in Regina's inner city.
(Photo by Trevor Hopkin)
Mosquito says that the ability to perform cultural activities such as beadwork and moss bags was lost as a result of residential schools. "The grandparents were the ones that were supposed to pass on the values and teach the kids," she says. "Now that piece is missing."
She sees her role at SEARCH as a way to bridge that gap. "We're trying to get all of that back, slowly … Even here."
As with the other mentors, Mosquito sees her job as providing services to both the clients and the student volunteers. "If you are wanting to teach or work in the North Central community, you need to know the cultural aspects of it and I'm always here to help answer those types of questions, not just for the clients that come in, but also for the students," she says. "So teaching people all of these protocols - how to dress, what to bring - it's all an important part of being here."
Kelly Husack BKin'15 is SEARCH's executive director. She also leads the Blue Dot Movement, an organization that advocates for a healthier environment. Husack first heard about SEARCH in Christian Thomson's Indigenous Studies 100 class at the First Nations University of Canada. She still remembers her first day at SEARCH. Following the SEARCH orientation session, she was nervously standing against the wall when one of the social workers approached her and said, "Jump in there and go have a conversation."
This invitation would alter the direction of Husack's life and fundamentally change her perspective on community health. After three years volunteering, and having entered her second year as executive director, Husack sees health as so much more than just offering treatment. She says that the community aspect SEARCH offers is its greatest remedy.
"We spend a lot of time with our clients," she says. "Often, needs that are presented on the medical side tend to be a lot more complex than just, 'I have a sore throat, etc.' There tends to be a lot more compounding factors, so we try to allow more time for that."
The Four Directions Community Health Centre in the North Central neighbourhood is home to SEARCH. The clinic has been offering primary health care in the community for more than 20 years.
(Photo by Trevor Hopkin)
Husack says that SEARCH helps lighten the load on the Regina health care system. "By coming here, people aren't utilizing emergency services, which reduces cost and strain on the emergency rooms at the main hospitals."
SEARCH also offers unique educational benefits to its student volunteers. "Students come in with their own backgrounds and their own sets of knowledge that they've gained through their university experience thus far," says Husack. "Then they get to meet and work with people in the community."
After years of working in interior design, Jessica Dunster BSNU'17 decided that it was time for a change. "I dealt with people that had lots of money to spend," says Dunster. "The materialism and the greed started to get to me."
That led Dunster to seek a career where she felt she could serve others. She quickly enrolled in a nursing program. It wasn't long into her program that Amanda Kukartz, SEARCH's previous director, came to her school on a student volunteer recruitment trip. Dunster had a choice of ten different placements and she chose SEARCH.
"I just felt that there was a lot of stigma to this area," says Dunster, "and as someone who was going into a health profession, I think that it was very important for me to understand the background that people from the inner city were coming from."
Jessica Dunster left a career in interior design for nursing in order to serve others.
(Photo by Trevor Hopkin)
Now a registered nurse at the General Hospital, Dunster says that her learning at SEARCH is something that you can't get in a classroom. "You can go and take an Indigenous health class and learn about the residential school system and everything that happened, but here you have the opportunity to sit down with someone and learn about their particular experience: what it has done to their family, what's going on now and the issues that that has caused."
"It was the individuals and families that I connected with that made it more personal for me," she says. "It kept me wanting to come back."
After completing her one-month course requirement, Dunster decided to continue volunteering. She eventually joined the student-led SEARCH Board of Directors and is now a board co-chair. "It was the individuals and families that I connected with that made it more personal for me," she says. "It kept me wanting to come back."
Dunster says that her time at SEARCH has opened her eyes to the judgement that marginalized people feel from our health care system, and, in turn, how she can become a better advocate. "Being at SEARCH has given me much more of a catalogue of contacts for help and supports that [marginalized] people can use."
Connecting with other students and professional mentors was also "huge" for her. She not only got to observe and perform pre-interviews with clients, but also to have key conversations with mentors about the clients' diagnoses.
Above all, Dunster says that SEARCH has helped her dig deeper and look beyond the clinical aspect of what's happening to people. And this, she says, has made her a better nurse. "It's made me more aware of getting to know what's going on in a person's life, so you can have more of an impact," she says. "It's having a more holistic approach. For some Indigenous people, this may mean getting them access to an Elder."
Dunster believes that without SEARCH, she would not have had the same depth of sensitivity to people-that she wouldn't be doing the same "digging" that she does now.
A black string with a large plastic white bat is wrapped snugly around the neck of Matthew Pechey BScHons'15, a second-year medical student and SEARCH volunteer. "I'm a fan of Batman," says Pechey. "I like to go to the Fan Expo in Regina-it's a good conversation starter."
Like Bruce Wayne, Pechey comes from a place of privilege. "I'm in a pretty advantaged situation as a Caucasian male coming from a middle-income family," says Pechey. "Acknowledging that lack of fairness and knowing that there's a responsibility to work towards something better is important, even if it's going to be slow and difficult."
Matthew Pechey, a second-year medical student and SEARCH volunteer.
(Photo by Trevor Hopkin)
Pechey speaks of the humility that he has learned as a SEARCH volunteer. "I am learning too. I might be doing one thing that I think is helpful, but then find out that it is completely inappropriate, that you need to be informed on what the specific needs are in the community rather than imposing your own prejudice."
Pechey first volunteered with SEARCH during his undergraduate degree in psychology. Seeing how the professional counselling mentors worked with clients and their family members was eye-opening. "[The mentors] have worked within the community and the insights they bring are very valuable," he says. "They know the events and the health care issues within this neighbourhood."
If Irene Mosquito is the wise SEARCH sage, then Sam Berg is the Jedi master. A veteran counsellor of more than 20 years, Berg's warm disposition is matched by his handsomely lined face and silver hair. "As mentors, we provide the services that we are professionally equipped to do and then we are observed," he says. "We then debrief after each session."
Berg says it's fascinating to watch the professional and educational progression of the students during their time at SEARCH. "It gives them the opportunity to get out of the ivory tower and get involved with people on the ground," he says. "It's been a really wonderful experience working with them and with the clients that come here as well."
Berg says that the students that come through SEARCH's doors give him hope for the future. "If there's a problem with millennials today, these aren't typical," he says with a laugh. "These are the type of people that get up in the morning, work hard and have dreams and ambitions."
Sam Berg a veteran counsellor and SEARCH volunteer.
(Photo by Trevor Hopkin)
One of those millennials is Aimee Kowallski, a second-year psychology student at the University of Regina and one of the ten people experiencing their first day at SEARCH. Like Kelly Husack, Kowallski first heard about SEARCH in Christian Thomson's Indigenous Studies 100 class. Originally from Moose Jaw, Kowallski says that the things she's been learning in her Indigenous studies class are "blowing her mind" and that she sees SEARCH as a great way to learn and help Regina become a better place.
Peter Boyko is a larger-than-life character. He is one of those rare people that can be loud and endearing at the same time. As soon as he rolled through the SEARCH doors, waves of smiles came over people's faces.
"I'm really happy this place is here," says Boyko.
Boyko has been coming to SEARCH for the past four years. While he's definitely used the medical and counselling services, Boyko makes it very evident that the staff and students here are his friends and that the social aspect of SEARCH is extremely important to him. He often refers to different staff members, such as Kay Yee (a dietician) and others as if they were his regular chums on coffee row at a small-town diner. "Chats with these people ranged from the efficacy of hydroelectricity, to the KKK, and then the limited uses of solar power," says Boyko.
A resident of Argyle Park, Boyko says he first noticed the Four Directions Centre when passing by on the bus. Now he doesn't know what he'd do without it. "I had an ear infection once, a cold another time. I saw the doctor a few times. I saw a counsellor when the social worker wasn't here," he says. "It's truly important that these [extended Saturday] hours are available."
Boyko brings up the sign that hangs above the kitchen in the main room. It says, 'Love is the best ingredient.' "It's not just a statement, but something that is lived out by the staff, and that includes those that come and volunteer on Saturdays," he says. "I'm really happy this place is here."
[post_title] => Regina’s SEARCH has the best ingredient
[post_excerpt] => Students are getting valuable health care mentoring by volunteering at a primary health care clinic.
[post_status] => publish
[comment_status] => open
[ping_status] => open
[post_password] =>
[post_name] => reginas-search-has-the-best-ingredient
[to_ping] =>
[pinged] =>
[post_modified] => 2022-02-24 14:24:58
[post_modified_gmt] => 2022-02-24 20:24:58
[post_content_filtered] =>
[post_parent] => 0
[guid] => https://www.degreesmagazine.ca/?p=1247
[menu_order] => 0
[post_type] => post
[post_mime_type] =>
[comment_count] => 0
[filter] => raw
)










 Graduating Cougars player, Charlotte Kot. (Photo by University of Regina Photography Department.)
There's a magic about this program - something that is difficult for alumni or coaches to put into words - but a wide variety of factors have come together to create a product that draws people to it, including recruits, top-level coaches and fans.
Graduating Cougars player, Charlotte Kot. (Photo by University of Regina Photography Department.)
There's a magic about this program - something that is difficult for alumni or coaches to put into words - but a wide variety of factors have come together to create a product that draws people to it, including recruits, top-level coaches and fans.
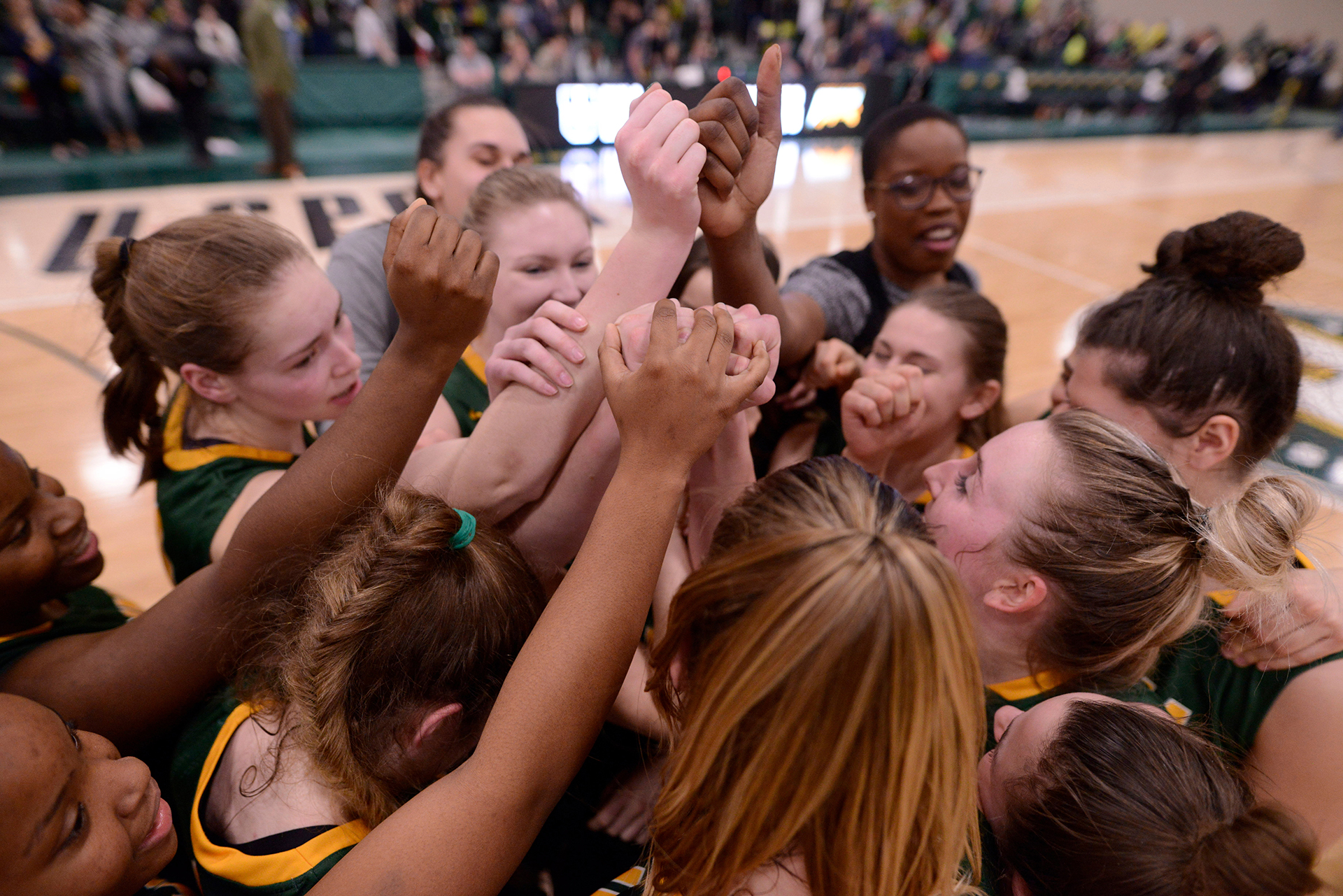 The Cougars celebrate another medal in a national championship, winning bronze at the 2018 USPORT tournament in Regina. (Photo by Arthur Ward)
Over the past 20 years, the Cougars have finished only one season without a winning record. This is a team that, since 1968, has played in the national university championship 19 times, advancing to the final championship game on six occasions. It is one of the best programs in Canada.
The success of the program can be attributed to a number of factors. Alumni and coaches have a slightly different view on what has advanced the program to the position sustained success it has seen. Perhaps it is the high calibre of local players developed through the Regina club and school programs. It could be the emphasis placed on recruiting. Or maybe it's simply the mindset of maintaining a high standard of excellence. Together, the elements have created a product that draws the support of the community and makes this one of the most respected programs in Canada.
The Cougars celebrate another medal in a national championship, winning bronze at the 2018 USPORT tournament in Regina. (Photo by Arthur Ward)
Over the past 20 years, the Cougars have finished only one season without a winning record. This is a team that, since 1968, has played in the national university championship 19 times, advancing to the final championship game on six occasions. It is one of the best programs in Canada.
The success of the program can be attributed to a number of factors. Alumni and coaches have a slightly different view on what has advanced the program to the position sustained success it has seen. Perhaps it is the high calibre of local players developed through the Regina club and school programs. It could be the emphasis placed on recruiting. Or maybe it's simply the mindset of maintaining a high standard of excellence. Together, the elements have created a product that draws the support of the community and makes this one of the most respected programs in Canada.
 Sue (McKenzie) Burns. (Photo by Trevor Hopkin)
The first year the team donned uniforms as the Cougettes was in 1968-69, playing for the University of Saskatchewan - Regina Campus under head coach Sheila Ward. Their green uniforms were made off-site, and the armholes were so small, the women couldn't raise their arms, says Irene Wallace, one of the original Cougette alumnus. "In the locker room after practice we ended up taking scissors and making larger arm holes so we could actually wear them."
Original Cougettes (left to right) Linda (Vail) Dodd BEd'74, Irene Wallace BEd'71, Ruby (Werhun) Patrick BEd'72 and and Laurie (Woods) Burgess BEd'70.
(Photo by Trevor Hopkin)
The developing history of Cougar women's basketball has continued to reflect the University, as it has grown from a completely local program to one that is recognized internationally.
Each head coach has continued to move the program forward. When Sue Higgs, a Department of Physical Education faculty member, began coaching the team in 1971, she began to revolutionize the team and women's sport.
"I think she was a little bit ahead of her time in terms of, let's take these young women and really maximize their physical potential, in addition to teaching us so many things we didn't know about the game," says Burns, who noted that they were always in the lab doing fitness testing as well as training off the court.
After Higgs' nine-year tenure, there were two losing seasons before Sheila (Brennan) Beckie was hired. A Regina product, she had played for the University of Saskatchewan, and brought with her enthusiasm for the program, as well as a real focus on recruiting local players.
"We were losing really good athletes out of the city," says Dick White CA'89, BEd'74, who worked for the University for 34 years, including 20 as athletic director. "One of her focuses was to keep the best Regina athletes here at the start."
Sue (McKenzie) Burns. (Photo by Trevor Hopkin)
The first year the team donned uniforms as the Cougettes was in 1968-69, playing for the University of Saskatchewan - Regina Campus under head coach Sheila Ward. Their green uniforms were made off-site, and the armholes were so small, the women couldn't raise their arms, says Irene Wallace, one of the original Cougette alumnus. "In the locker room after practice we ended up taking scissors and making larger arm holes so we could actually wear them."
Original Cougettes (left to right) Linda (Vail) Dodd BEd'74, Irene Wallace BEd'71, Ruby (Werhun) Patrick BEd'72 and and Laurie (Woods) Burgess BEd'70.
(Photo by Trevor Hopkin)
The developing history of Cougar women's basketball has continued to reflect the University, as it has grown from a completely local program to one that is recognized internationally.
Each head coach has continued to move the program forward. When Sue Higgs, a Department of Physical Education faculty member, began coaching the team in 1971, she began to revolutionize the team and women's sport.
"I think she was a little bit ahead of her time in terms of, let's take these young women and really maximize their physical potential, in addition to teaching us so many things we didn't know about the game," says Burns, who noted that they were always in the lab doing fitness testing as well as training off the court.
After Higgs' nine-year tenure, there were two losing seasons before Sheila (Brennan) Beckie was hired. A Regina product, she had played for the University of Saskatchewan, and brought with her enthusiasm for the program, as well as a real focus on recruiting local players.
"We were losing really good athletes out of the city," says Dick White CA'89, BEd'74, who worked for the University for 34 years, including 20 as athletic director. "One of her focuses was to keep the best Regina athletes here at the start."
 Sue Higgs began coaching the team in 1971 and began to revolutionize the team and women's sport. (Photo courtesy of University of Regina Archives and Special Collections.)
During her first season, there was such a lack of returning players and few players previously recruited that Beckie would have to join the players in practice to have enough bodies. Then, she successfully recruited Jackie Moore BPAS'91 of Thom Collegiate. The Cougars continued to improve, winning the Great Plains Athletic Conference (GPAC) final and going to the national championship in the 1988-89 season.
Sue Higgs began coaching the team in 1971 and began to revolutionize the team and women's sport. (Photo courtesy of University of Regina Archives and Special Collections.)
During her first season, there was such a lack of returning players and few players previously recruited that Beckie would have to join the players in practice to have enough bodies. Then, she successfully recruited Jackie Moore BPAS'91 of Thom Collegiate. The Cougars continued to improve, winning the Great Plains Athletic Conference (GPAC) final and going to the national championship in the 1988-89 season.
 The 2000-01 CIS championship women's CIS team. (Photo by University of Regina Photography Department)
As the Cougars became more successful, their fan base also grew. In 1999, the Cougars were playing the University of Manitoba in the best-of-three GPAC final. After the warmup, Stapleton and Taylor were walking toward the team room, about 40 feet down the hallway from the gym, and could hardly get through because the lineup to the gym was out the door. "Dave and I looked at each other, with big smiles on our faces, and were like, 'Can you believe this?' " says Stapleton.
Jeff Speedy, who was hired as the head coach in 2002 after Stapleton, says the city's passion for the program makes Regina one of the top places in the country to coach. "It's a special place to play, it's a special place to coach, and it's a very special program," he says.
The 2000-01 CIS championship women's CIS team. (Photo by University of Regina Photography Department)
As the Cougars became more successful, their fan base also grew. In 1999, the Cougars were playing the University of Manitoba in the best-of-three GPAC final. After the warmup, Stapleton and Taylor were walking toward the team room, about 40 feet down the hallway from the gym, and could hardly get through because the lineup to the gym was out the door. "Dave and I looked at each other, with big smiles on our faces, and were like, 'Can you believe this?' " says Stapleton.
Jeff Speedy, who was hired as the head coach in 2002 after Stapleton, says the city's passion for the program makes Regina one of the top places in the country to coach. "It's a special place to play, it's a special place to coach, and it's a very special program," he says.
 Former Cougars player Cymone (Bouchard) Bernauer. (Photo by University of Regina Photography Department)
The next year, the team was creating new memories in a state-of-the-art facility after the Centre for Kinesiology Health and Sport opened. They needed to win the third game in the series to advance to the final four. The Cougars had graduated three players the previous year, one being Bernauer, who had been named the CIS Player of the Year. "We were trailing late in the game," says Speedy. "We were down six points with only five minutes left in the game, and I can still remember Jana (Schweitzer) Linner BAdmin'05, and Leah Anderson taking the game over. Basically, they were just saying, 'There's no way our careers are done today.' We won that game to even the series, and won the next day to go back to the final four."
The move to the new 2,400-seat gym meant a beautiful new team room, additional training facilities and, later, a jumbotron.
"It changed the atmosphere a little bit," says Maja Kralcacova BKin'09, who played for the Cougars from 2003 to 2009. "But it also gave the opportunity for a lot more people to watch us play."
Maja Kralcacova.
(Photo by Trevor Hopkin)
Kralcacova was one of the first international players to come to Regina. Originally from Prague in the Czech Republic, Kralcacova played her senior year of high school in Macklin, Saskatchewan, before Speedy recruited her to the Cougars.
"The team is now kind of reflecting where the U of R's going," says De Ciman. "Internationalization is growing, and you can almost say it's mirroring the University."
While the Regina community supports its local players, it also welcomes international players, making them feel like family.
"It was just incredible how people embraced me. … It was really nice, and that continued throughout all of my years," says Kralcacova, who stayed in Regina following her basketball career and recently became a Canadian citizen.
The warm welcome is because of avid fans like Gord Staseson, who Kralcacova now calls her "grandpa" for all he has done for her over the years.
"He took me under his wing, and started to help me fundraise money for Adopt-a-Cougar," says Kralcacova, who remains close friends with Staseson. "He actually raised money to bring my mom here for the (2009) CIS Championship, which was really touching, and I will never forget it."
Former Cougars player Cymone (Bouchard) Bernauer. (Photo by University of Regina Photography Department)
The next year, the team was creating new memories in a state-of-the-art facility after the Centre for Kinesiology Health and Sport opened. They needed to win the third game in the series to advance to the final four. The Cougars had graduated three players the previous year, one being Bernauer, who had been named the CIS Player of the Year. "We were trailing late in the game," says Speedy. "We were down six points with only five minutes left in the game, and I can still remember Jana (Schweitzer) Linner BAdmin'05, and Leah Anderson taking the game over. Basically, they were just saying, 'There's no way our careers are done today.' We won that game to even the series, and won the next day to go back to the final four."
The move to the new 2,400-seat gym meant a beautiful new team room, additional training facilities and, later, a jumbotron.
"It changed the atmosphere a little bit," says Maja Kralcacova BKin'09, who played for the Cougars from 2003 to 2009. "But it also gave the opportunity for a lot more people to watch us play."
Maja Kralcacova.
(Photo by Trevor Hopkin)
Kralcacova was one of the first international players to come to Regina. Originally from Prague in the Czech Republic, Kralcacova played her senior year of high school in Macklin, Saskatchewan, before Speedy recruited her to the Cougars.
"The team is now kind of reflecting where the U of R's going," says De Ciman. "Internationalization is growing, and you can almost say it's mirroring the University."
While the Regina community supports its local players, it also welcomes international players, making them feel like family.
"It was just incredible how people embraced me. … It was really nice, and that continued throughout all of my years," says Kralcacova, who stayed in Regina following her basketball career and recently became a Canadian citizen.
The warm welcome is because of avid fans like Gord Staseson, who Kralcacova now calls her "grandpa" for all he has done for her over the years.
"He took me under his wing, and started to help me fundraise money for Adopt-a-Cougar," says Kralcacova, who remains close friends with Staseson. "He actually raised money to bring my mom here for the (2009) CIS Championship, which was really touching, and I will never forget it."
 Gord Staseson (Grandpa to former player Maja Kralcacova) hoods her at her 2009 convocation ceremony. (Photo courtesy of Maja Kralcacova)
Much of the recruiting to the Cougars, however, still remains within the city. Regina minor level and high school basketball teams continue to develop strong athletes who grow up wanting to play for the Cougars. Alumni give their time generously, coaching at various levels as they become role models in the community.
"I think we have always had the perfect storm," says Taylor. "We've been successful. Our players are great ambassadors out in the community. So there's that connection. … Local will always be the foundation of our program. The minute that changes, we're in trouble."
Thirteen years after joining the Cougar women's basketball team as an assistant coach, Taylor was made head coach in 2006.
"It's a village that builds this program," says Stapleton, noting the athletic directors, deans of Kinesiology and Health Studies, and University presidents who have supported the teams and shown up to games. "And it's a guy like Dave, who has arguably the longest tenure of anybody associated with the women's basketball program."
Taylor is quick to acknowledge the coaches that came before him as the team's builders, while he says he is committed to maintaining that excellence as guardian of the program.
For most of the past 25 years, the University of Regina women's basketball program has been in the capable hands of Dave Taylor or Christine Stapleton.
(Photo by Rae Graham)
"There have been all these moments and times where I thought there were tipping points that could have gone either way. Oftentimes, it has been having the right player with the right mindset," says Taylor, in looking back on the team's success over the years. "The players have had that competitive drive and ownership, and just pursuit of excellence where anything less is just not acceptable."
In 2013-14 and 2014-15, the Cougars had back-to-back seasons where injuries became a huge issue, leading to two seasons where the team didn't go to nationals. The summer of 2015, Charlotte Kot became the team's heartbeat, and her drive to succeed permeated the entire team. "Everybody had that attitude of, 'Okay, enough. We can't be 500. This is not acceptable,' " says Taylor. "And now, we're back on a three-year run of being in the Canada West finals."
While players like Kot will certainly never forget playing in a national championship, she says her most important memories of the weekend were not on the court. Instead, she will remember the alumni who returned for the weekend, including those such as Andrea (Gottselig) Ward and Amy (Mickleborough) Moroz, who co-chaired the 2018 championship committee.
"The thing I will remember the most about that nationals was all of the alumni," says Kot, who was awed by the packed gym watching the alumni game and the lunch with over 65 alumni present. "The people change, but they are always your family. … Once a Cougar, always a Cougar."
Crystal (Heisler) McGregor played with the Cougars from 1996-2002. Her death from cancer in 2014 brought players closer together than they had ever been.
Never was this more apparent than when Crystal (Heisler) McGregor was diagnosed with cancer in 2012. McGregor played for the Cougars from 1996 to 2002. The Cougar alumni - including both her teammates and those from teams before and after - came together to fundraise and help McGregor in her battle against cancer. When she died in 2014, they began the Crystal McGregor Memorial Scholarship in her memory.
"It drew us closer together than we've ever been, and that's the beauty of being part of a team," says Bernauer. "No matter what happens to somebody in that extended family, we all pull together, and we all show up for support."
"As tragic as it was to lose Crystal, you try to answer the question 'why?' We tried to take the love and the positive out of it," says Ward. "Crystal reconnected all alumni in a deeper and more meaningful level of team than ever before."
Gord Staseson (Grandpa to former player Maja Kralcacova) hoods her at her 2009 convocation ceremony. (Photo courtesy of Maja Kralcacova)
Much of the recruiting to the Cougars, however, still remains within the city. Regina minor level and high school basketball teams continue to develop strong athletes who grow up wanting to play for the Cougars. Alumni give their time generously, coaching at various levels as they become role models in the community.
"I think we have always had the perfect storm," says Taylor. "We've been successful. Our players are great ambassadors out in the community. So there's that connection. … Local will always be the foundation of our program. The minute that changes, we're in trouble."
Thirteen years after joining the Cougar women's basketball team as an assistant coach, Taylor was made head coach in 2006.
"It's a village that builds this program," says Stapleton, noting the athletic directors, deans of Kinesiology and Health Studies, and University presidents who have supported the teams and shown up to games. "And it's a guy like Dave, who has arguably the longest tenure of anybody associated with the women's basketball program."
Taylor is quick to acknowledge the coaches that came before him as the team's builders, while he says he is committed to maintaining that excellence as guardian of the program.
For most of the past 25 years, the University of Regina women's basketball program has been in the capable hands of Dave Taylor or Christine Stapleton.
(Photo by Rae Graham)
"There have been all these moments and times where I thought there were tipping points that could have gone either way. Oftentimes, it has been having the right player with the right mindset," says Taylor, in looking back on the team's success over the years. "The players have had that competitive drive and ownership, and just pursuit of excellence where anything less is just not acceptable."
In 2013-14 and 2014-15, the Cougars had back-to-back seasons where injuries became a huge issue, leading to two seasons where the team didn't go to nationals. The summer of 2015, Charlotte Kot became the team's heartbeat, and her drive to succeed permeated the entire team. "Everybody had that attitude of, 'Okay, enough. We can't be 500. This is not acceptable,' " says Taylor. "And now, we're back on a three-year run of being in the Canada West finals."
While players like Kot will certainly never forget playing in a national championship, she says her most important memories of the weekend were not on the court. Instead, she will remember the alumni who returned for the weekend, including those such as Andrea (Gottselig) Ward and Amy (Mickleborough) Moroz, who co-chaired the 2018 championship committee.
"The thing I will remember the most about that nationals was all of the alumni," says Kot, who was awed by the packed gym watching the alumni game and the lunch with over 65 alumni present. "The people change, but they are always your family. … Once a Cougar, always a Cougar."
Crystal (Heisler) McGregor played with the Cougars from 1996-2002. Her death from cancer in 2014 brought players closer together than they had ever been.
Never was this more apparent than when Crystal (Heisler) McGregor was diagnosed with cancer in 2012. McGregor played for the Cougars from 1996 to 2002. The Cougar alumni - including both her teammates and those from teams before and after - came together to fundraise and help McGregor in her battle against cancer. When she died in 2014, they began the Crystal McGregor Memorial Scholarship in her memory.
"It drew us closer together than we've ever been, and that's the beauty of being part of a team," says Bernauer. "No matter what happens to somebody in that extended family, we all pull together, and we all show up for support."
"As tragic as it was to lose Crystal, you try to answer the question 'why?' We tried to take the love and the positive out of it," says Ward. "Crystal reconnected all alumni in a deeper and more meaningful level of team than ever before."